October 1918. The war in Europe was nearly over. On the North Shore of Long Island — along the stretches of Route 25A that would later become the roads I know best — towns like Stony Brook, St. James, Smithtown, and Port Jefferson were small communities of farmers, tradesmen, and the families of men who had shipped out to France. Nobody had antibiotics. Nobody had a ventilator. Nobody understood viruses, not really. What they had were linen strips, camphor, whiskey, and whatever room in a church or general store they could clear out fast enough.
The pandemic that tore through the world between 1918 and 1920 infected an estimated 500 million people — roughly a third of the planet’s population at the time — and killed somewhere between 50 and 100 million of them. In the United States alone, more than 675,000 died. More Americans died from the Spanish flu than in all of World War I, World War II, Korea, Vietnam, Iraq, and Afghanistan combined. Life expectancy in the U.S. dropped by more than twelve years in a single year. When Southold Town historian Amy Folk described the coffin shortage to the Suffolk Times, she didn’t reach for metaphor: “They ran out of coffins. They were stacking them up like cords of wood.”
The Ground It Came From
The virus didn’t announce itself. It arrived the way most catastrophes do — quietly at first, dressed as something ordinary. The first confirmed case in New York City came via the port on August 14, 1918, when a Norwegian steamship arrived at the harbor carrying ill passengers and crew. By September, influenza had been added to the list of reportable diseases. By October, 9,000 people would die in New York City in a single month. One resident recalled watching neighbors drop: “The deaths were so sudden it was unbelievable. You would be talking to someone one day, and hear about his death the next day.”
What made the 1918 strain uniquely terrifying wasn’t just its speed. It defied the pattern that epidemiologists expected. Influenza typically kills the very young and the very old. This virus killed healthy people between twenty and forty — the exact cohort of men and women who were running farms, staffing the local general store, raising children, building houses along the North Shore’s back roads. Early autopsies described lungs weighing six times their normal weight, filled with a thin, bloody froth. Patients turned blue. They literally drowned in their own fluids.
John Barry, author of The Great Influenza, put it plainly in a presentation to the Virginia Historical Society: “There were reports from Eskimo villages in Alaska and jungle villages in the middle of Africa of 100% mortality. In 1918, society began to dissolve.”

Camp Upton and What Spilled Out
Long Island didn’t just feel the pandemic from a distance. It was one of the first places in the country where the second, far more lethal wave hit the ground. Camp Upton — a military training installation near Yaphank, on land that is now Brookhaven National Laboratory — became a catastrophe zone before most of the civilian population understood what was coming.
The story of how it arrived at Upton is grim. The virus had broken out at Camp Devens in Massachusetts, killing 757 soldiers. Before a proper quarantine could be imposed, a contingent of replacement troops was moved from Devens directly to Camp Upton. The disease arrived at Upton on September 13, 1918. Four days later, 171 of the camp’s 43,000 soldiers were hospitalized. By October 5, there were 4,371 cases and twenty men died in a single day.
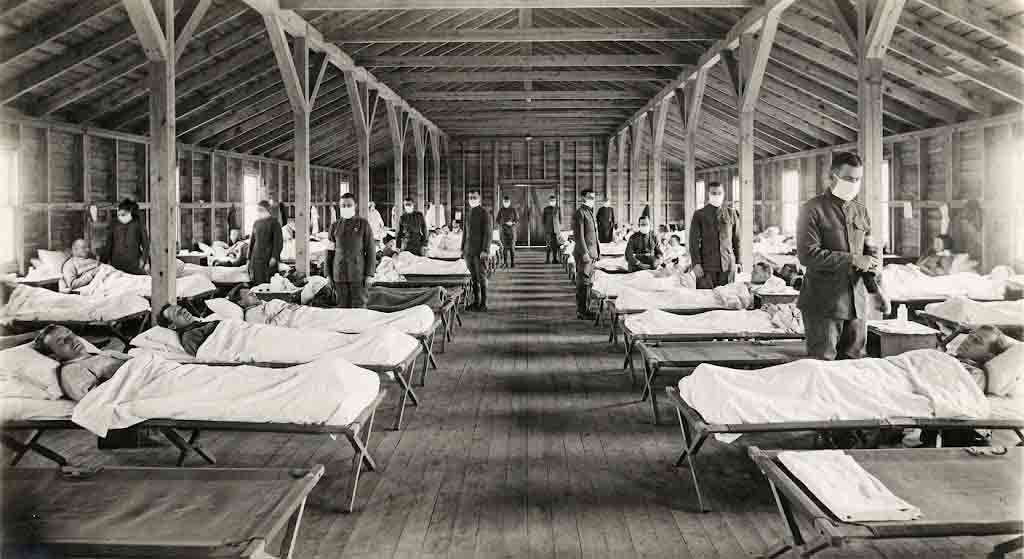
Camp commander Colonel John Mallory locked the installation down — no civilian visitors, no leaves — and ordered soldiers to wear gauze masks and sit on opposite sides of mess tables. When the camp’s post hospital was overwhelmed, medical officers converted any available structure into temporary wards. Sheets were hung between beds. The Journal of the American Medical Society recorded officers’ “horror at the frightfulness of the sight of the hopelessly sick and dying and at the magnitude of the catastrophe.” By the time Upton’s epidemic was declared over on October 22, 6,131 soldiers had been hospitalized and 404 had died. One of them, Private James Down, entered the hospital on September 23 with a fever of 104 degrees and died three days later. An Army pathologist preserved a section of his lung in wax and sent it to the Army Medical Museum — a specimen that, in 1999, would help researchers at the Armed Forces Institute of Pathology identify exactly what made the 1918 virus so lethal.
The virus did not stay inside the camp’s perimeter.
What a Small Town Does With No Hospital
The Three Village area — Setauket, Stony Brook, and Old Field — sat directly in the shadow of what was unfolding at Upton. Suffolk County had no major hospital infrastructure capable of absorbing a catastrophic surge of respiratory patients. What it had were community buildings, private homes, church halls, and the kind of neighbor-to-neighbor resourcefulness that rural communities had always relied on when the government infrastructure ran out.
Across Long Island, the story repeated in every town. Schools were closed. Movie theaters and houses of worship shut down. Buildings that had served as community gathering spaces were cleared and converted. Private homes took in the sick when nowhere else was available. Families were decimated — not metaphorically, but literally, with multiple members dying within days of each other. The shortage of coffins became a practical crisis.
Physicians and nurses worked until they collapsed. With so many doctors and nurses deployed to the war effort, civilian medical personnel were stretched past any reasonable limit. Drug stores gouged prices. Snake oil sellers moved through communities peddling fraudulent cures. Meanwhile, legitimate public health measures — staggered business hours, gauze masks, house-to-house canvassing for unreported cases — were rolled out across New York with varying effectiveness.
The first mention of the Spanish Influenza in a Long Island newspaper came in July 1918 in the South Side Signal of Babylon, reporting that 80 percent of Spain’s population had been infected. By September, the North Fork had its first reported case — Milton Hallock of Riverhead, a Navy serviceman being treated in New London, Connecticut. The disease had no respect for geography or social standing. Irving E. Smith of Sayville, reported to be among the earliest Suffolk County fatalities from the virus, died in France in October 1918 while on service. His body wasn’t returned to the United States for four years.
What They Used to Fight It
The medical response to the 1918 pandemic should be understood against one hard fact: nobody knew what caused it. Germ theory was established, but viruses had not been identified as a distinct category of pathogen. Influenza was thought to be caused by a bacterium. There was no vaccine. There were no antivirals. There were no antibiotics to treat the secondary bacterial pneumonia that killed most patients after the flu had already weakened them.
What communities had were public health tools borrowed from older campaigns against tuberculosis and cholera: quarantine, isolation, ventilation, sanitation. New York City Health Commissioner Royal Copeland had built much of his response on lessons learned from tuberculosis control — house-to-house case canvassing, mandatory reporting, emergency health district coordination. He kept the city’s schools open and resisted theater closures, a decision that drew fierce criticism from the Red Cross of Long Island and former health commissioner Dr. S.S. Goldwater, who publicly called the in-school inspection program one of “almost criminal laxity.”
Research conducted decades later for the CDC would validate the critics: cities that responded early, sustained their interventions, and deployed multiple tools simultaneously — school closures, canceled gatherings, isolation and quarantine — showed meaningfully lower mortality rates than those that did not. The timing mattered enormously. Howard Markel, a physician and historian at the University of Michigan, summarized it plainly: “Cities that reacted early and in a sustained way using more than one of those three options did better in terms of mortality than those that did not.”
On the ground, improvised treatments included carbolic acid gargle solutions, chlorinated soda rinses, and experimental antiseptic sprays applied directly to the nasal passages. At Camp Upton, medical officers sprayed the throats of 800 healthy men daily with a dichloramine-T solution in hopes of preventing spread — a measure that proved ineffective but reflected the desperation of a medical community working without the tools to identify, let alone defeat, what it was fighting.
What Vanished From the Record
The pandemic ended, roughly speaking, by 1920. The Roaring Twenties roared right over it. Prohibition was now law. Jazz was coming north. People were tired of death. They chose to forget, the way people always choose to forget when the crisis passes and normal life reassembles itself.
That collective amnesia has a specific shape when you look at North Shore Long Island. The military records of Camp Upton are relatively well-documented — the Army kept careful statistics, as armies do. But the civilian record of what happened in the small communities along Route 25A, in the farm towns and fishing villages of the North Fork, in the back rooms of general stores and the pews of churches that were cleared of their benches and filled with cots — that record is fragmentary and difficult to reassemble. Local newspapers from the period are scattered. Death certificates exist but require archival excavation. The oral histories are almost entirely gone.
What survives is this: the pandemic killed more than 675,000 Americans in roughly two years. It tore through Suffolk County as it tore through every American county. The community response — improvised, under-resourced, and ultimately effective enough that the population did not collapse — was built on neighbor helping neighbor, on repurposed buildings, on gauze and whiskey and the stubbornness of people who had no other option.
We were already here, already building this place. And we came through it without any of the tools we would one day take for granted. That’s worth remembering.
If you’re interested in how prohibition-era Long Island navigated another kind of lawlessness, my piece on Rum Row and the Freeport Bootleggers covers how the North Shore dealt with the 1920s on its own terms. And for more on how this stretch of road has shaped our history, see The Ride Down 25A.
Sources
- The Suffolk Times: “When the Spanish Flu Struck in 1918 and Its Impact Here”
- U.S. Army: “Worldwide Flu Outbreak Killed 45,000 American Soldiers During World War I”
- New York State Division of Military & Naval Affairs Press Release on Camp Upton
- PMC: “The U.S. Military and the Influenza Pandemic of 1918–1919”
- PMC: “The 1918 Influenza Epidemic in New York City: A Review of the Public Health Response”
- National Endowment for the Humanities: “The Devastation of 1918”
- Tenement Museum: “The Flu of 1918: Sneeze but Don’t Scatter”
- NYC Department of Records: “The Flu Epidemic of 1918”
- Stanford University: “The 1918 Influenza Pandemic: Response”
- Barry, John M. The Great Influenza: The Story of the Deadliest Pandemic in History. Viking, 2004.







