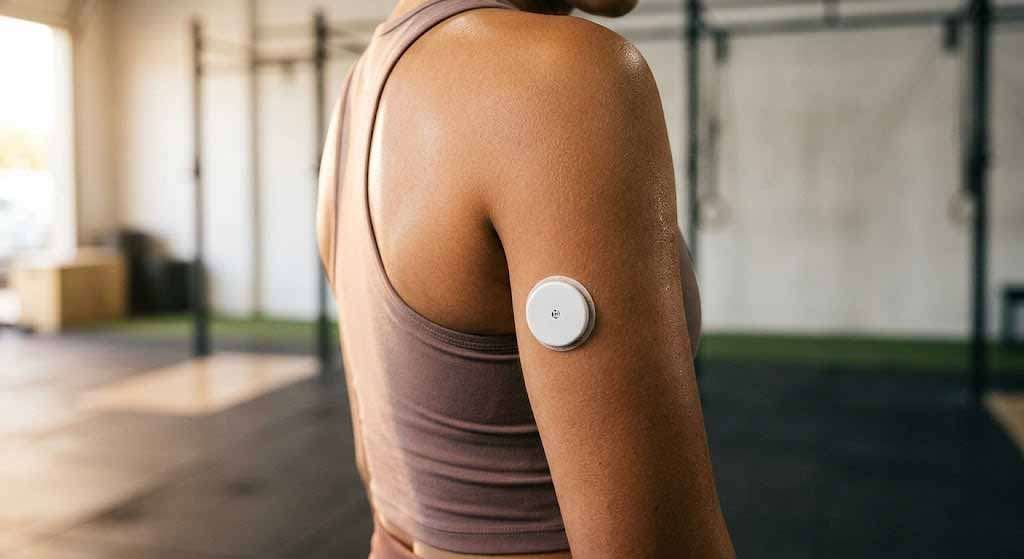
A quarter-inch filament sits under the skin of your upper arm. It measures glucose in the interstitial fluid every five minutes and sends the number to your phone. No finger prick. No blood. No waiting for a lab to call you back three days later with a fasting number that tells you almost nothing about how your body actually processes the food you eat. That filament — and the device attached to it — was built for people with diabetes. It was never supposed to end up on the arm of a thirty-four-year-old CrossFit coach in Setauket who eats clean and runs a 6:20 mile. But here we are.
Continuous glucose monitors, or CGMs, have crossed the line from medical necessity to metabolic curiosity. And what they’re revealing is making a lot of people rethink everything they thought they knew about carbs, timing, and what “healthy eating” actually means for their specific body.

What a CGM Actually Does
A continuous glucose monitor is a small wearable sensor — roughly the size of two stacked quarters — that gets applied to the back of the upper arm with a spring-loaded applicator. A thin, flexible filament inserts just beneath the skin into the subcutaneous tissue, where it measures glucose concentrations in the interstitial fluid. That reading gets transmitted via Bluetooth to a smartphone app, generating a continuous stream of data that plots your glucose levels across hours, days, and weeks.
The technology was originally developed for Type 1 diabetics who needed real-time visibility into their blood sugar to manage insulin dosing. Companies like Dexcom and Abbott (makers of the FreeStyle Libre) built these devices to prevent dangerous hypoglycemic and hyperglycemic episodes — the kind that send people to emergency rooms. For that population, CGMs have been transformative. They replaced the old routine of finger-prick testing six or eight times a day with a passive, 24-hour data stream that could integrate directly with insulin pumps.
But somewhere around 2022, the devices started showing up in places nobody at Dexcom’s engineering lab had anticipated. Endurance athletes. Biohackers. Wellness influencers. Keto dieters. And then, increasingly, regular people who just wanted to know why they crashed every day at 2 PM despite eating what they were told was a balanced lunch.
The Data That Changes the Conversation
The most disruptive thing about CGMs isn’t the technology. It’s the information.
For decades, nutritional science has operated on population-level generalizations. Whole grains are good. Fruit is healthy. White rice spikes your blood sugar. Oatmeal stabilizes it. These broad guidelines have some truth in them, but they treat every human metabolism as interchangeable. A CGM makes that assumption impossible to maintain.
What users consistently discover — and what clinical researchers have been documenting — is that postprandial glucose responses (the spike your blood sugar takes after eating) vary wildly between individuals eating the exact same food. One person eats a banana and stays flat at 95 mg/dL. Another person eats the same banana and rockets to 160. One person handles white rice without a blip. Another person’s glucose graph after a bowl of brown rice looks like they ate a candy bar.
A landmark 2015 study out of Israel’s Weizmann Institute, published in Cell, tracked 800 participants using CGMs and found that individual glycemic responses to identical foods were so variable that standardized dietary recommendations were essentially useless for predicting any one person’s reaction. The researchers built machine learning models that could predict individual responses based on gut microbiome composition, meal timing, sleep, and physical activity — and those personalized models outperformed every existing dietary guideline.
That study cracked something open. It gave scientific credibility to what biohackers and athletes had been saying anecdotally: your body is not a textbook, and the only way to know how it handles food is to measure it directly, in real time.

Why Athletes and CrossFitters Got There First
Elite athletes are obsessive about fuel. They have to be. A marathon runner who bonks at mile 18 because their glycogen stores depleted too early lost the race not in their legs but in their nutrition strategy. A CrossFit competitor who crashes mid-WOD because they ate the wrong pre-workout meal two hours before knows — viscerally — that timing and composition matter at a granular level.
CGMs gave these athletes something no food diary or macro tracker could: a real-time feedback loop. Eat something. Watch the curve. Learn. Adjust. Repeat. Research from the Gatorade Sports Science Institute, drawing on data from over 7,500 athletic CGM users wearing Abbott Libre sensors, found that roughly 80 percent of glucose readings in healthy athletes fell between 70 and 140 mg/dL, but about 17 percent of readings exceeded 140 — a number that would concern most doctors on a fasting glucose panel. Elite endurance athletes, in particular, showed significant glucose variability during high-carbohydrate fueling windows around training, with spikes well above 140 mg/dL that were entirely normal and functional in context.
The takeaway isn’t that those spikes are dangerous. It’s that glucose behavior during training, recovery, and rest is far more dynamic and individual than anyone assumed. And without a CGM, none of that data existed. You were flying blind.
Companies like Levels, Nutrisense, and Signos spotted this demand early and built direct-to-consumer platforms that paired CGM hardware with coaching apps, food-logging tools, and AI-driven metabolic scoring. They turned a clinical device into a consumer product. And the market responded.
The Dexcom Stelo: The Over-the-Counter Turning Point
In March 2024, the FDA cleared the Dexcom Stelo — the first over-the-counter continuous glucose monitor in U.S. history. No prescription. No diabetes diagnosis. No telehealth visit required. Just a sensor, an app, and your arm.
The Stelo uses the same core technology as the clinical-grade Dexcom G7, but it’s configured for wellness users rather than insulin-dependent patients. It tracks glucose trends, identifies spikes and dips, and provides daily and weekly summaries — but it doesn’t include the medical-grade alarms and insulin-pump integration that diabetic patients rely on. It costs roughly $89 to $99 per month for a two-sensor pack, each sensor lasting 15 days. It’s HSA and FSA eligible.
Abbott followed with its own pair of clearances in June 2024: the Lingo, designed for general wellness consumers, and the Libre Rio, aimed at Type 2 diabetics not on insulin. The wellness CGM market had officially arrived.
For Long Islanders, this means you can walk into a pharmacy — or order from Amazon — and have a continuous glucose monitor on your arm by tomorrow. No gatekeeping. No insurance dance. No waiting room. The device that used to require a specialist’s prescription is now sitting next to the Fitbits and Apple Watches in the health aisle.
What the Numbers Actually Mean (and What They Don’t)
Here’s where it gets important, and where the hype machine needs a check.
A healthy, non-diabetic person’s fasting glucose typically sits between 70 and 100 mg/dL. After a meal, glucose rises — that’s normal physiology — and in most people, it returns to baseline within about two hours. The general target for non-diabetic CGM users is to keep glucose between 70 and 140 mg/dL for the vast majority of the day, a metric called “time in range.” Research suggests that healthy adults spend about 96 percent of their time in that window.
But a spike to 150 after a plate of pasta doesn’t mean you’re pre-diabetic. It means you ate a plate of pasta. The danger comes when spikes are frequent, prolonged, and don’t resolve — patterns that indicate insulin resistance, which is the metabolic dysfunction that precedes Type 2 diabetes, often by years. A CGM can reveal those patterns long before they show up on an annual fasting glucose test, and that’s where the real preventive value lives.
The flip side is worth stating plainly: if you’re a healthy person without metabolic dysfunction, you can become anxious watching numbers fluctuate that were never meant to stay flat. A 2025 Mass General Brigham study found that CGM metrics in people without diabetes did not reliably correlate with HbA1c — the gold standard for long-term blood sugar control. The researchers cautioned that people with normal glycemic control should be careful about drawing clinical conclusions from CGM data alone.
That’s a real concern. The glucose number on your phone is a datapoint, not a diagnosis. It becomes powerful when you use it to observe patterns over weeks — how sleep affects your fasting levels, how a 20-minute walk after dinner flattens your post-meal curve, how stress at work creates glucose spikes that have nothing to do with food. It becomes counterproductive when you treat every bump on the graph as a crisis.
How Long Islanders Can Access CGMs Without a Diabetes Diagnosis
The access landscape has shifted dramatically. Here’s where things stand:
The Dexcom Stelo is available over-the-counter at major retailers and directly from Dexcom’s website. No prescription needed. At roughly $89 per month on subscription, it’s the most accessible entry point for anyone curious about their glucose patterns.
For those who want more than raw data — coaching, meal scoring, dietitian consultations — subscription platforms like Nutrisense, Levels, and Signos bundle CGM hardware with app-based analytics and professional guidance. Prices range from around $129 to $199 per month depending on the plan length and features. Most include a telehealth consultation that handles any prescription requirements for clinical-grade sensors.
HSA and FSA accounts can cover CGM purchases in many cases, which softens the out-of-pocket cost considerably. If you’re already using those accounts for gym memberships, supplements, or other wellness spending, a CGM fits right into that category.
Talk to your doctor, too. A growing number of primary care physicians and endocrinologists on the North Shore are familiar with CGM use in non-diabetic patients, particularly for patients showing early signs of insulin resistance, PCOS, or metabolic syndrome. The conversation is no longer unusual.
The Bigger Picture: Personalized Metabolic Data as the New Standard
Fitness trackers gave us step counts and heart rate. Sleep trackers gave us REM cycles. CGMs give us something fundamentally different — a window into how our metabolism processes the single most important variable in our diet: glucose. That window is personal, continuous, and immediate. It doesn’t rely on population averages or nutritional dogma. It shows you what your body does, in your body, in real time.
The technology isn’t perfect. The science for healthy populations is still catching up to the consumer market. And no sensor on your arm replaces a physician who understands your full clinical picture. But the direction is clear. We’re moving from a world where metabolic data was available only to the sick, toward one where anyone who wants to understand their own biology can do so for less than the price of a monthly gym membership.
That shift — from reactive medicine to proactive self-knowledge — is the real revolution. The glucose monitor is just the instrument.
You Might Also Like:
- NoCo — 429 North Country Road, St. James, NY 11780
- Per Se — 10 Columbus Circle, 4th Floor, New York, NY 10019
- Harbor Mist — 105 Harbor Road, Cold Spring Harbor, NY 11724
Sources:
- Zeevi, D., et al. “Personalized Nutrition by Prediction of Glycemic Responses.” Cell, 2015. https://www.cell.com/cell/fulltext/S0092-8674(15)01481-6
- Shah, V.N., et al. “Continuous Glucose Monitoring Profiles in Healthy Nondiabetic Participants.” Journal of Clinical Endocrinology & Metabolism, 2019.
- Gatorade Sports Science Institute. “Continuous Glucose Monitoring Use in Athletes Without Diabetes.” https://www.gssiweb.org/sports-science-exchange/article/continuous-glucose-monitoring-use-in-athletes-without-diabetes
- Klonoff, D.C., et al. “Use of Continuous Glucose Monitors by People Without Diabetes: An Idea Whose Time Has Come?” Journal of Diabetes Science and Technology, 2023. https://pmc.ncbi.nlm.nih.gov/articles/PMC10658694/
- Rodriguez, J.A., et al. “Lack of Association Between Hemoglobin A1c and Continuous Glucose Monitor Metrics among Individuals with Prediabetes and Normoglycemia.” Diabetes Technology and Therapeutics, 2025. https://www.massgeneralbrigham.org/en/about/newsroom/press-releases/continuous-glucose-monitoring-for-people-without-diabetes
- Dexcom Stelo. https://www.stelo.com
- Nutrisense. https://www.nutrisense.io
- Levels Health. https://www.levels.com
- Signos. https://www.signos.com