Fear is a fantastic marketing tool. Sell someone a problem they didn’t know they had, then sell them the solution. The keto world has a version of this that’s become so embedded in online culture that even smart, biology-literate people repeat it without checking: eat too much protein and your body converts it to glucose, which spikes insulin, which kicks you out of ketosis. Neat, tidy, and mostly wrong. The real biochemistry behind gluconeogenesis — what it actually is, who controls it, and why your ribeye isn’t the enemy — is one of the most misunderstood topics in low-carb nutrition. Time to straighten it out.
What Gluconeogenesis Actually Is
Gluconeogenesis (GNG) is the liver’s process of synthesizing glucose from non-carbohydrate precursors — amino acids, lactate, glycerol, and pyruvate. It is ancient, conserved across virtually every vertebrate, and absolutely essential for survival. Without it, your brain — which can run on ketones but not exclusively — would have no glucose buffer during fasting, sleep, or prolonged exertion. GNG is not a metabolic accident triggered by eating too much steak. It is a tightly regulated baseline process that runs continuously, regardless of what you ate for dinner.
The confusion begins when people treat GNG as if it were a simple overflow drain: pour in excess protein, and glucose pours out the other side. The body doesn’t work that way. GNG is primarily governed by demand signals — cortisol, glucagon, epinephrine — not by substrate availability. The liver does not simply convert amino acids to glucose because they’re present. It converts them because the organism needs glucose right now, and dietary carbohydrate isn’t supplying it.
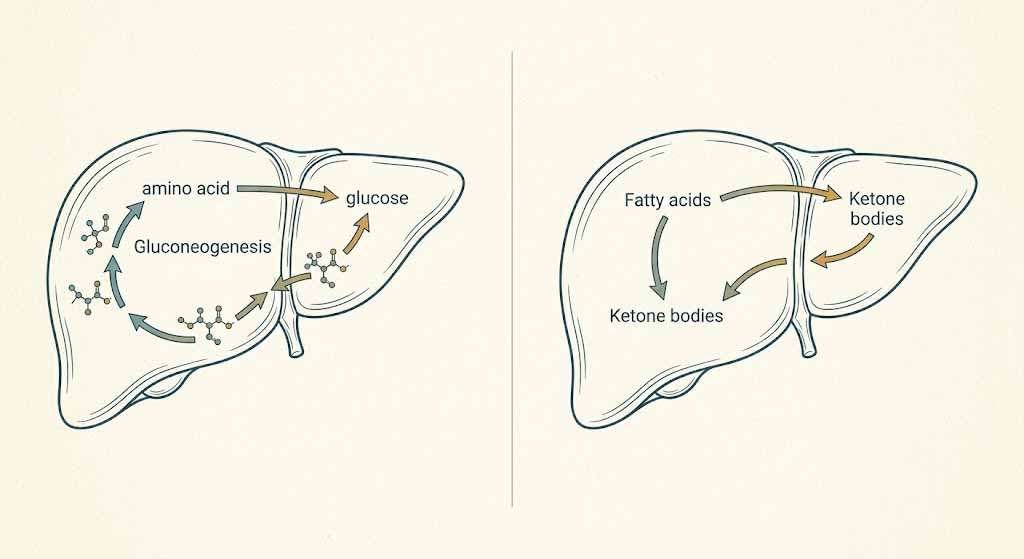
Demand-Driven vs. Supply-Driven: The Distinction That Changes Everything
This is the core of the argument, and it’s worth being precise. Demand-driven GNG is what the body does all the time on a ketogenic diet. Glucose-dependent tissues — red blood cells, the renal medulla, parts of the brain — require a steady trickle of glucose that ketones cannot replace. The liver obliges, pulling mostly from lactate and glycerol rather than amino acids, and produces just enough glucose to meet those requirements. Ketosis is not disrupted because the glucose produced is immediately consumed by tissues that literally cannot use ketones. The system is in balance.
Supply-driven GNG — the kind the protein-fear crowd is worried about — would require the liver to upregulate glucose production in response to an amino acid surplus, even when demand is already met. The evidence for this happening to any meaningful degree in healthy humans eating moderate-to-high protein on a ketogenic diet is thin. A 2015 study published in Cell Metabolism by Kevin Hall and colleagues found that protein intake well above typical recommendations did not meaningfully increase glucose production or impair ketosis in subjects adapted to a low-carbohydrate diet. The liver, in the presence of adequate ketones and suppressed insulin, does not go rogue.
Think of it like water pressure in a well-engineered pipe system. The pump only runs when the pressure drops below a set threshold. You can add more water to the reservoir — more amino acids available — but if the pressure is already adequate, the pump doesn’t spin up. The regulator controls the output, not the input volume.

The Insulin Response to Protein: Smaller Than You Think, Faster Than It Matters
Here’s where the myth picks up its second leg: even if GNG doesn’t flood you with glucose, protein triggers an insulin response, and insulin kills ketosis. This one has a kernel of truth buried inside a misleading framing.
Yes, protein — particularly leucine-rich proteins like whey — does stimulate insulin secretion. This is not a bug. It’s a co-regulated response: protein also stimulates glucagon, the hormone that does the opposite of insulin in glucose metabolism. The simultaneous rise of both insulin and glucagon in response to a protein meal is a well-documented phenomenon sometimes called the protein paradox, and it results in net-neutral glucose dynamics. Insulin rises enough to drive amino acid uptake into muscle tissue (anabolism — the whole point), while glucagon prevents hypoglycemia by maintaining hepatic glucose output. The net effect on blood glucose is minimal. The net effect on ketosis in an adapted individual is, for most people, negligible.
The insulin spike from a protein-rich meal is both smaller in magnitude and shorter in duration than the insulin response to equivalent carbohydrate consumption. Comparing the two and treating them as interchangeable is like comparing the wake of a rowboat to a ferry crossing and concluding they both sink docks. The magnitudes matter. The adaptation timeline for keto is part of the reason some people see more disruption early on — before the metabolic machinery is fully tuned to fat oxidation, any insulin signal feels more consequential than it actually is.
Why the Myth Persists — and Who It Serves
Bad science doesn’t survive in a vacuum. It survives because it serves someone’s interest, fills an anxiety, or confirms a pre-existing belief. The “too much protein will kick you out of ketosis” myth does all three.
It serves supplement companies selling “pure fat” products — MCT oil, fat bombs, keto meal replacements — that would lose their appeal if people understood that high-protein, moderate-fat approaches work just as well for most people. It fills the anxiety of the tracking-obsessed, who need something concrete to optimize and worry about, and protein intake is an easy numerical target. And it confirms the framework of a small but vocal corner of the keto community that has elevated dietary fat to near-religious status, treating any deviation as apostasy.
The truth is more pragmatic and less marketable: protein is satiating, muscle-preserving, thermogenic, and among the most effective single dietary variables for body composition on any eating pattern. On a ketogenic diet, adequate protein — even generous protein — does not reliably impair ketone production in individuals who are otherwise eating very low carbohydrate. The research on the protein leverage hypothesis actually suggests the opposite problem is more common: people undereating protein, triggering compensatory overeating of everything else.
What Actually Kicks You Out of Ketosis
Since we’re being honest about the biochemistry, let’s be equally honest about the real culprits. Dietary carbohydrate — especially rapidly absorbed simple sugars — raises insulin sharply and durably enough to suppress fatty acid mobilization and halt ketone production. Alcohol, which the liver prioritizes as a metabolic substrate above everything else, effectively pauses fat oxidation for the duration of its clearance. Chronic stress, via cortisol, drives gluconeogenesis upward and insulin resistance with it. Severe sleep deprivation has measurable effects on glucose regulation and insulin sensitivity.
None of these are the grilled chicken breast. None of these are the dozen eggs. The ribeye you’re eating for dinner — grass-fed, properly sourced, the way a keto diet was built to accommodate — is not your problem. The problem is the hidden maltodextrin in your “keto” bar, the two glasses of wine you’re not counting, and the four hours of sleep you’re getting because you’re too busy reading forums about protein macros at midnight.
How Much Protein Is Actually Appropriate
Current evidence supports protein intakes well above the old-guard keto recommendations for most active adults. The 0.6–0.8 grams per pound of body weight figure that circulated for years was borrowed from sedentary population averages and applied wholesale to people lifting weights and trying to maintain lean mass during a fat-loss protocol. It was always too conservative. Research from groups including Layne Norton, Donald Layman, and others working in protein metabolism and body composition suggests that intakes of 1.0–1.2 grams per pound of lean mass are reasonable targets for active individuals — and that these intakes do not undermine ketosis in subjects maintaining low carbohydrate intake.
For practical purposes: eat enough protein to protect your muscle, satisfy your appetite, and support your training. Keep carbohydrates genuinely low — that’s the actual lever for ketosis. And stop listening to people who built a supplement brand on top of your fear of chicken thighs. The biochemistry doesn’t support them. Your grocery bill shouldn’t either.
If you’re still calibrating your approach to keto eating on Long Island, the North Shore Keto Diner Survival Guide covers the practical side of staying on protocol when you’re eating out — without having to stress the macros into a spreadsheet before every meal.
You Might Also Like
- The Ketogenic Adaptation Timeline: What Actually Happens to Your Metabolism in Weeks 1–12
- Protein Leverage Hypothesis: Why Your Body Might Be Tricking You Into Overeating Carbs
- The Best Cuts of Meat for Keto—and How to Cook Each One
Sources
- Hall KD, et al. “Calorie for Calorie, Dietary Fat Restriction Results in More Body Fat Loss than Carbohydrate Restriction in People with Obesity.” Cell Metabolism, 2015. https://doi.org/10.1016/j.cmet.2015.07.021
- Nuttall FQ, Gannon MC. “Metabolic response of people with type 2 diabetes to a high protein diet.” Nutrition & Metabolism, 2004. https://doi.org/10.1186/1743-7075-1-6
- Norton L, Layman D. “Leucine Regulates Translation Initiation of Protein Synthesis in Skeletal Muscle after Exercise.” Journal of Nutrition, 2006. https://doi.org/10.1093/jn/136.2.533S
- Layman DK. “Protein quantity and quality at levels above the RDA improves adult weight loss.” Journal of the American College of Nutrition, 2004. https://doi.org/10.1080/07315724.2004.10719380
- Volek JS, Phinney SD. The Art and Science of Low Carbohydrate Performance. Beyond Obesity LLC, 2012.






